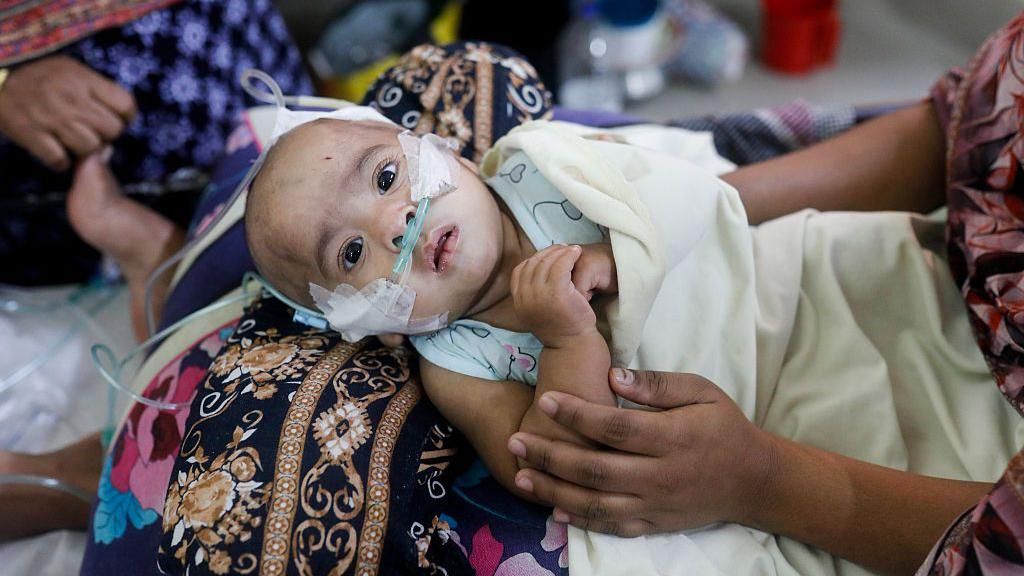
In the quiet graveyard of Taunsa, a city in Pakistan’s Punjab province, 10-year-old Asma kneels beside the fresh grave of her 8-year-old brother Mohammed Amin. Amin died in agonizing pain after testing positive for HIV, his fevers so severe that he begged to sleep in cold rain, his body twisting in torment “like he had been thrown into boiling oil”, recalls his mother Sughra. Today, Asma carries the same virus that killed her brother – a diagnosis that has upended her childhood, even as Sughra herself has tested negative for HIV.
Asma and Amin are not isolated tragedies. An 11-month investigation by BBC Eye has documented a large-scale HIV outbreak among children in Taunsa, with at least 331 minors testing positive for the virus between November 2024 and October 2025. The overwhelming majority of these cases cannot be linked to mother-to-child transmission: of 97 infected children whose families received testing, just four of their mothers tested positive. Public health data explicitly lists contaminated needles as the transmission route for more than half of all confirmed cases, pointing to unsafe medical practices at Taunsa’s government-run Tehsil Headquarter (THQ) Hospital as the source of the outbreak.
Local private physician Dr Gul Qaisrani first sounded the alarm in late 2024, after he noticed a sharp spike in pediatric HIV cases passing through his clinic. Nearly 70 of the children he diagnosed had received routine care at THQ Taunsa, he says. Multiple families told Qaisrani that hospital staff reused single-use syringes across multiple children, including one account of a syringe used for an HIV-positive cousin that was then reused for other patients. One father reported confronting nursing staff over the dangerous practice, only to be ignored.
In response to growing public pressure, Punjab provincial authorities promised a “massive crackdown” on unsafe practices in March 2025, and suspended THQ Taunsa’s then-medical superintendent Dr Tayyab Farooq Chandio. But BBC Eye can reveal that Chandio was back treating children within three months, working as a senior medical officer at a rural health center on Taunsa’s outskirts. In an interview, Chandio denied the hospital was the source of the outbreak, claiming he took all required safety measures as soon as the first case was identified.
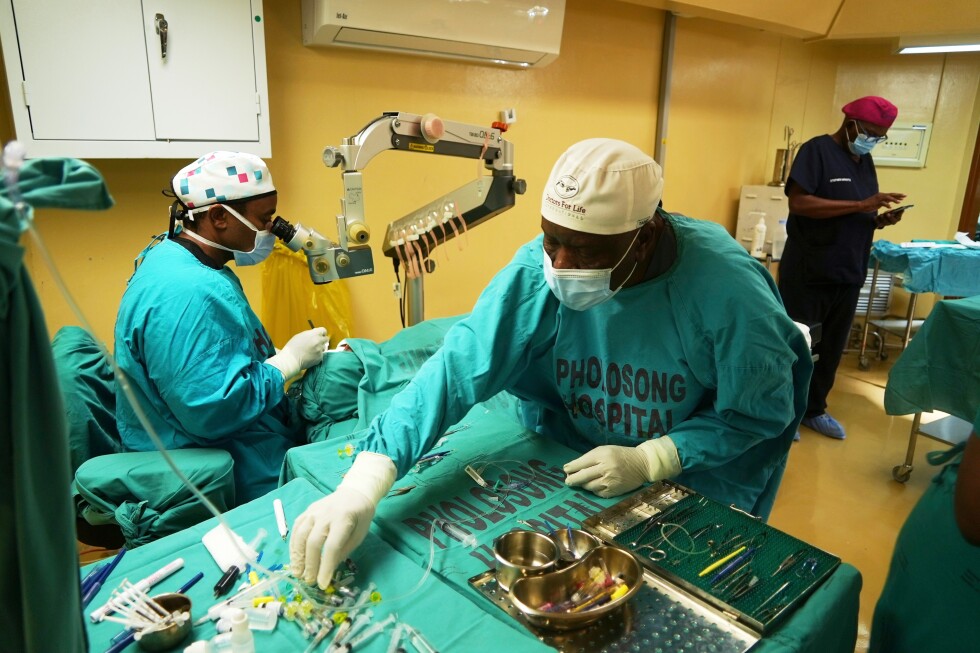
Chandio’s replacement, Dr Qasim Buzdar, took over in March 2025 and promised a “zero tolerance” policy for unsafe infection control, saying he had implemented mandatory training for all hospital staff on safe injection practices. But 32 hours of undercover filming conducted by BBC Eye at THQ Taunsa in late 2025 – eight months after the government’s intervention – exposes that dangerous, infection-spreading practices remained rampant.
The undercover footage captures 10 separate instances of staff reusing syringes to access multi-dose medicine vials, a practice that contaminates the entire vial’s contents. In four of these cases, medicine from the contaminated vial was then administered to other children. While it is unknown whether any of the patients involved were HIV-positive, infectious disease experts confirm that this creates a direct, high risk of viral transmission. “Even if they attach a new needle, the body of the syringe retains the virus, so transmission will still occur,” explained Dr Altaf Ahmed, a leading Pakistani microbiologist and infectious disease consultant, after reviewing the footage.
The investigation also documented widespread failures in basic infection control: over the filming period, 66 instances of medical staff – including at least one doctor – administering injections without wearing sterile gloves were captured. One nurse was filmed rummaging through a medical waste disposal bin with bare hands, a violation of every core principle of safe medical practice, Ahmed notes. Used injection equipment was left out on non-sterile countertops alongside open vials of medication, and one nurse was filmed pulling a used syringe with leftover patient liquid from under a counter and passing it to a colleague for reuse.
When presented with the footage, Buzdar refused to acknowledge its authenticity, claiming either that it was recorded before he took office or that it was staged. He insisted to BBC Eye that THQ Taunsa is a safe facility for children, telling local parents: “I can say with certainty and confidence that you should get your treatment done here.” The local government echoed this position, stating that no validated epidemiological evidence has conclusively linked THQ Taunna to the outbreak, and pointing to unregulated private care and unscreened blood transfusions as potential contributing factors. But a leaked April 2025 joint inspection report from UNICEF, the World Health Organization, and Pakistan’s regional health department reached conclusions that align with BBC Eye’s findings: the report specifically flagged dangerous conditions in THQ Taunsa’s pediatric emergency department, noting missing essential medications, widespread unsafe injection practices, poor hand hygiene, and reused intravenous equipment.
Health experts say the ongoing risks at THQ Taunsa are not isolated failures, but the product of deep systemic flaws in Pakistan’s public health system. Pakistan has one of the highest rates of unnecessary therapeutic injections in the world, driven by both public demand and provider习惯 that prioritize injections over oral medication for mild conditions. A chronic shortage of medical supplies, paired with quota-based allocation of equipment to government hospitals, also incentivizes dangerous cost-cutting like syringe reuse. “They have a fixed number of supplies to last an entire month, so corner-cutting becomes inevitable, even when it puts patients at deadly risk,” explained Dr Fatima Mir, a professor of pediatrics at Karachi’s Aga Khan University Hospital.
This is not the first time such systemic failures have led to a large pediatric HIV outbreak in Pakistan. In 2019, over 1,500 children tested positive for HIV in Ratodero, Sindh province, in an outbreak that was also linked to reused syringes in public health facilities; new infections continue to be recorded there today. More recently, an 84-case outbreak of pediatric HIV in Karachi’s SITE Town area was publicly confirmed by Pakistan’s federal health minister to have been caused by syringe reuse at the local government-run Kulsoom Bai Valika Hospital, despite the facility’s superintendent denying such practices could occur.
When contacted about BBC Eye’s findings, a spokesperson for Pakistan’s national government said it had acted promptly to investigate concerns and roll out updated infection control guidelines to all health facilities in March 2025.
For the families affected by the Taunsa outbreak, however, these policy changes come too late. Asma now faces a lifetime of HIV treatment, her health already declining as she loses weight unexpectedly. She faces deep social isolation from HIV-related stigma: neighborhood parents bar their children from playing with her, leaving her lonely as well as sick. She often asks her mother, “What is wrong with me?”
Standing at her brother’s grave, Asma says she misses him every day. “He’s with God now,” she says. Despite the pain and uncertainty of her future, she still holds onto a dream: “I work hard at school. When I grow up, I want to become a doctor.”