ZIMBABWE has emerged as a pioneering nation in the global fight against HIV/AIDS by launching a groundbreaking twice-yearly preventive injection that promises to transform prevention strategies for vulnerable populations. The revolutionary drug lenacapavir, administered just semiannually, represents a significant advancement over daily oral PrEP medications that have long posed adherence challenges for high-risk groups.
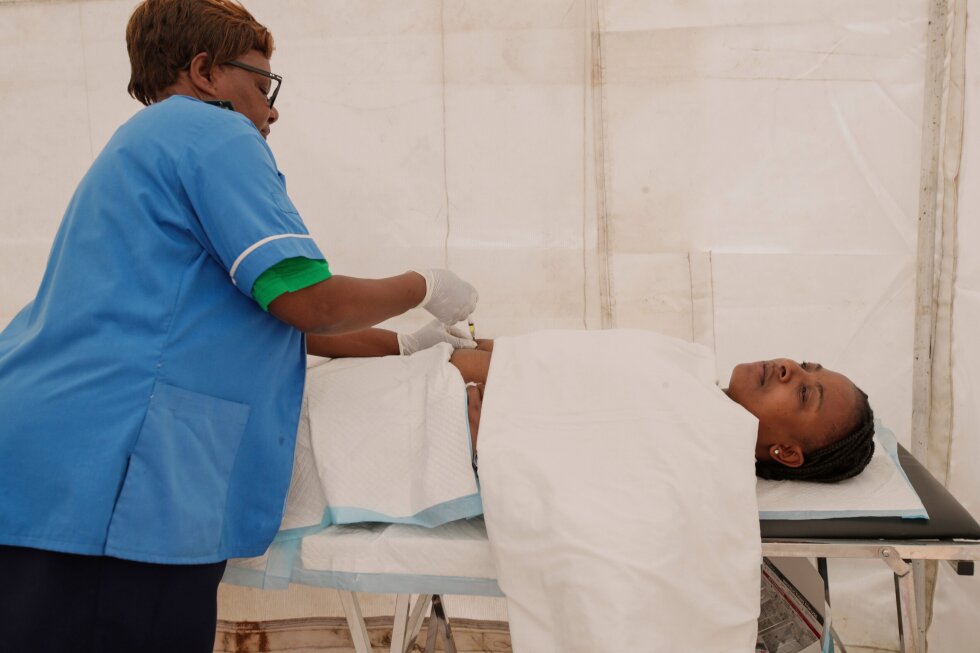
At a dedicated rollout event in Harare’s outskirts, diverse beneficiaries including sex workers, young mothers, and LGBTQ+ individuals received their initial injections in mobile clinic settings. The atmosphere reflected both hope and relief among recipients who have struggled with the practical limitations of existing prevention methods.
Developed by California-based pharmaceutical innovator Gilead Sciences, this long-acting injectable demonstrates near-total protection efficacy in clinical trials. The African rollout across ten nations including Zimbabwe, Zambia, and Eswatini receives substantial support through PEPFAR (President’s Emergency Plan for AIDS Relief) in collaboration with the Global Fund.
Health Minister Douglas Mombeshora emphasized the transformative potential during the launch ceremony: ‘Effective prevention must integrate seamlessly into real lives. When health solutions prove overly complex, demanding, or visibly stigmatizing, compliance inevitably suffers. Lenacapavir fundamentally reimagines our approach to HIV prevention.’
Despite Zimbabwe’s remarkable progress in epidemic control—achieving WHO testing, treatment, and viral suppression targets—new infections persist concerningly among adolescent girls and young women. UN data reveals HIV prevalence among sub-Saharan African females aged 10-24 remains persistently triple that of male counterparts, driven by structural inequalities and healthcare access disparities.
Practical implementation challenges loom large, however. With each injection costing approximately $54 annually per person even at negotiated nonprofit pricing, sustainable scaling remains financially constrained for many African governments. Health infrastructure limitations and diminishing foreign aid further complicate widespread accessibility.
Medical professionals stress that lenacapavir should complement rather replace existing prevention tools. ‘Condoms remain essential—they’re affordable and prevent additional sexually transmitted infections,’ noted Enerst Chikwati of AIDS Healthcare Foundation.
For early recipients like Constance Mukoloka, a 27-year-old sex worker, the injection already delivers profound impact: ‘This means security and professional confidence. Daily pills created client suspicion and scheduling difficulties. Now I can work without compromising protection for six months.’