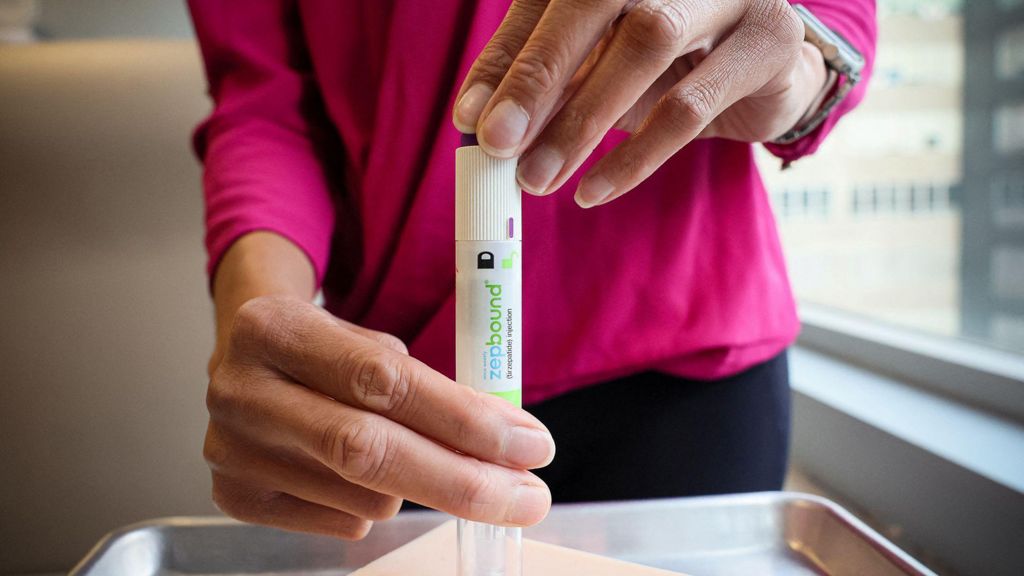
The American pharmaceutical market is witnessing an unprecedented price competition in the weight-loss medication sector, creating both opportunities and challenges for patients seeking treatment. The landscape has evolved dramatically since Eli Lilly’s Zepbound entered the market at over $1,000 per monthly dose in 2023, with current prices now starting at $299 for self-paying customers.
This transformative shift stems from manufacturers adopting direct-to-consumer strategies amid widespread insurance coverage gaps. Major pharmaceutical companies have bypassed traditional distribution channels by establishing online sales platforms and partnering with retail giants like Walmart and Costco. The competitive pressure has intensified as manufacturers contend not only with each other but also with a legally operating off-label industry that emerged during medication shortages.
Ruth Gonzalez’s experience exemplifies this changing dynamic. The 56-year-old self-employed professional initially restructured her entire budget—switching phone plans, eliminating streaming services, and cutting discretionary spending—to afford Zepbound’s $350 monthly cost. Her sacrifices yielded significant health benefits: normalized blood pressure within six weeks and a 40-pound weight reduction that addressed her sleep apnea and fatty liver disease concerns. The subsequent price reductions enabled her to advance to more effective dosage levels while anticipating future pill-based alternatives.
However, the market transformation presents a dual reality. While prices have dropped substantially—Novo Nordisk’s Wegovy now costs $149 monthly for self-pay patients compared to its original $1,600 price point—these medications remain financially inaccessible for many Americans. Shekinah Samayah-Thomas, a 62-year-old California resident, exemplifies the ongoing coverage crisis. Despite undergoing bariatric surgery and struggling with weight recurrence, she lost Medicaid coverage for Wegovy in January and cannot afford continued treatment even with manufacturer coupons.
The political dimension adds complexity to this healthcare evolution. The Trump administration’s TrumpRx website promotes direct manufacturer relationships for select medications, while Medicare’s planned trial coverage of weight-loss drugs beginning July 2024 could pressure private insurers to follow suit. Health advocates maintain cautious optimism, recognizing that market competition provides temporary solutions but comprehensive insurance coverage remains the ultimate objective for ensuring equitable access to obesity treatments.
Experts emphasize that while transparent pricing models challenge the traditional pharmacy benefit manager system, most patients will still benefit more from insurance coverage than direct purchases. The coming years may bring further price reductions as patents expire and new formulations enter the market, but fundamental systemic reforms remain necessary to address America’s pharmaceutical affordability crisis comprehensively.