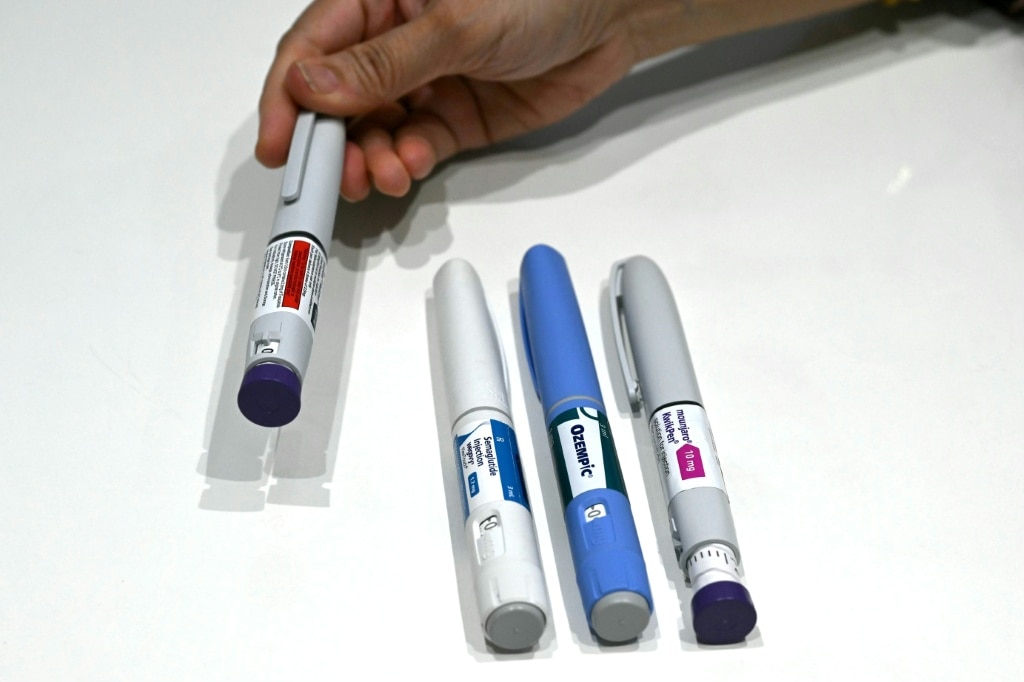
A seismic shift is underway in global obesity treatment as India’s pharmaceutical industry prepares to launch affordable generic versions of breakthrough weight-loss injections following the expiration of key patents. The expiration of semaglutide patents—the active component in medications like Ozempic and Wegovy—on Friday has unlocked unprecedented opportunities for mass production of cost-effective alternatives.
Medical facilities across Mumbai are already anticipating a substantial surge in patient demand. Endocrinologist Nadeem Rais reports approximately 50 weekly inquiries for weight-loss injections at his clinic alone, with current patient numbers ranging between 70-80. “With generic availability and subsequent price reductions, this figure could easily escalate to 200,” Dr. Rais projected.
The timing coincides with India’s evolving health crisis where traditional undernutrition challenges now compete with rapidly rising obesity rates. Recent government data reveals 24% of women and 23% of men are classified as overweight or obese—a paradoxical development in a nation that still accounts for one-third of global undernutrition cases.
India’s pharmaceutical giants have positioned themselves at the forefront of this transformation. Regulatory documents confirm at least four major manufacturers have prepared generic semaglutide formulations, with Zydus Lifesciences announcing immediate “Day 1” launches. Market research firm Pharmarack anticipates an influx of more than 50 brands from over 40 manufacturers entering the market shortly.
The economic implications are substantial. India’s weight-loss medication market has experienced tenfold growth over five years, reaching $153 million in 2026 with projections exceeding $500 million by 2030. Current premium treatments costing 15,000-22,000 rupees ($161–$236) monthly have limited accessibility, but generics are expected to reduce costs to approximately 5,000 rupees ($60) monthly.
This development carries significant global ramifications, particularly for middle-income nations where obesity rates are climbing but treatment remains cost-prohibitive. As the supplier of over half of Africa’s generic medications, India’s affordable semaglutide could become a vital resource for developing regions.
Medical professionals acknowledge both the promise and challenges. While these medications demonstrate remarkable efficacy, they can produce side effects including nausea and gastrointestinal discomfort. Nonetheless, as bariatric surgeon Sanjay Borude observes, the treatment addresses a growing health crisis fueled by sedentary urban lifestyles and changing economic patterns.